 Trust your instincts. Know your value. I recently moved due to my health (all my chronics), and due to some additional health issues that resulted after a car accident that totaled my car. I am a chronic pain warrior, a mental health warrior, and by training a special education teacher, early interventionist, tutor, and Certified Fibromyalgia Coach (and other chronic disorders too). Due to my chronics, I had to stop working in 2012. I also stopped working then as my supervisor was incredibly abusive and I wasn’t being backed up by the administration. I had my first in-person job in June of 2019 at one of the best, most supportive preschools I have worked in, with the most amazing staff, and I’ve worked in many. I was in a new city and things just kept happening to me. I was injured multiple times, burned by scalding water from a bottle warmer, and the ultimate was on June 10, 2020. I was in a car accident and there are parts of it I didn’t remember how I got from where I was to the crash site (which wasn’t a far distance at all but still scary). Thank G-d, I have an amazing mom who hired someone to drive the 10 hours from where I lived to where she was. She found doctors who could help me better than anyone I had been to in that city where someone of the top healthcare workers reside. With G-d's help, I’m healing and found a permanent residence here, a place I never thought I’d live again. I want to get back to my two points above. Trust your instincts and know your value. I had to switch insurances living in a new state and not only had difficulty finding one for me but once I did, I found very few who took it. I had an initial Telehealth appointment with a doctor and he nearly turned me into a blubbering mess. I’m on meds for my various conditions and he lectured me on that. He told me the treatments I was doing were of no use and that I should have stood up for myself. All of this over Zoom and I couldn’t say anything but “I’m sorry” over and over. I felt like I was being disciplined by a parent which (in real life) didn’t happen often because I was and still am a people pleaser. I got off that call feeling worthless, stupid and so much more. I then reached out to my support system who helped me realize that I wasn’t wrong, that this man was, and he clearly did not know me nor my body, to make the drastic changes he wanted me to make. After several discussions with friends, family and healthcare providers, this past saturday night, I sent him an email highlighting what he did to me and how it made me feel. I then canceled our next appointment and asked never to be contacted by him or his staff ever again. And now I’m looking for another person that took me 2 months to find and am hoping to change my health insurance as well. As fellow spoonies, I imagine you have been in similar situations or even worse. Do not doubt your knowledge of your disorders and do not let your medical professional berate, break you down, and destroy you. Have your information and enter that meeting strong and confident. Only you gets to choose how you want to care for your body. Only you can choose the doctors and other professionals in the healthcare field that are best for you. People can help guide you (like me! - shameless plug ;) ) to help get you into the right direction. I’m working hard every day to continue to strengthen myself from the inside out. When you grew up with a parent who was often disappointed with you because you had an LD that was not diagnosed until the summer before 12th grade, being lectured like that stirs up some major PTSD. I’ve grown a backbone, for the most part, but this “doctor” stripped me of it for a short time. Why just a picture of my eyes? Well, someone once said that your eyes are the gateway to your soul. I'm not sure how I feel about that statement. But, I strongly dislike having my picture taken and while the photographer was taking pictures of me and my family, I allowed him to only show my eyes. I am very expressive even in a nonverbal way. I believe when you look into those/my eyes, you can see how I'm feeling. I’m not/never looking for pity. Remember, no one has control over you but YOU. Do not let anyone make you think you are less than you actually are. Work on being proud of what you are and what you can do. I work on that daily. If you need help with this, please reach out.
0 Comments
 It’s been about two and a half years since my last blog post and my only reason is...life. A big move, lots of medical issues, COVID, a car accident, and am now in the middle of another big move (related to the accident and completely unplanned). During most points of this section of time, even opening a blank page to start a blog intimidated me and made me anxious. I usually write when I’m feeling this way, but not this time. But, here we are. I want to talk to you about this amazing invention called the “Zero Gravity Beanbag” made by a company called Zero Gravity Zen. I learned about this small company unconventionally, but am so glad I did! I follow a couple of YouTube families and they all fall under the same vein of raising children and young adults with disabilities. One of these YouTube pages, which I highly recommend, by the way, is called Six Blind Kids. The videos recount the life of parents, who after having one biological child, found themselves unable to conceive again. So, they begin adopting and within a matter of years, they adopted six blind kids, most with other developmental delays as well. I truly enjoy the videos and learning about each child/young adult and how they became part of the family and what they contribute to the family as they all do. I also found out about the Zero Gravity Beanbag as it was featured in one of their videos. As someone with chronic pain, I wondered if this might help me since I need to change positions so often to be comfortable and not become stiff and cause pain. I reached out to the owner, Keith, just to learn more about the beanbag and the cost. I expected a longer description and a price tag. Instead, I had an offer (with no requirement to write about it) to have it sent to me free to try it out with no expectation for its return. A huge box appeared on the porch one day and I brought it into the living area and opened it up. This bag came to me quickly and I was eager to try it out. It looked huge. Now, I’m petite (I *like* to say I’m 5’2”) but in no way small. I sent a barrage of emails to Keith with questions about how to use it the right way and he kindly answered each one personally. On the website, the beanbag is described as a “Zero Gravity Zen Bag For Stress Relief In Calming & Comfort.” To me, that is the absolute perfect description. The product specs are: Weight: 10 lbs Filling Material: High-Density Polystyrene (Foam) Mini Beads Outer Cover: Poly/Cotton Twill & Lycra/Spandex top for added comfort Removable cover for easy washing. This beanbag will literally retain most shapes you try. My favorite is to have my head up higher for reading and my feet out straight. And because I am “height-challenged,” my feet barely hang over the other edge. The foam beads move easily even while on the beanbag. I have yet to find an “uncomfortable” position. It takes the weight off my back and I can be on it for hours without accumulating pain when I would in/on other pieces of furniture. I wouldn’t quite call this furniture; but, it’s super comfy that I’ve even napped on it (and if you know me at all, napping is quite difficult). This beanbag is nearly perfect for those of us with chronic pain conditions/chronic illnesses with only one small complaint. For those of you that have trouble getting up and down from the floor, you may need to place this beanbag near something you can grab onto to pull yourself up (or do more core work, but the first idea is more likely for us “spoonies”). I do have to roll over to get off the bag but I don’t struggle too much to get up off my hands and knees thanks to the yoga I try to do on a semi-regular basis (meaning once a week - it’s made a HUGE difference but that’s another topic). So, if it’s not nice outside (although they have an outdoor version of this), you can find me on this beanbag with a weighted blanket and a nice book or reading/playing games on my iPad. I can lay on this for hours without ANY discomfort. Now, as I stated, I got this free and the upfront cost is high but to be honest, if I had tried someone else’s for a couple of hours, the cost would be worth it. (Again, this is not a paid promotion or even a requested promotion from/for the company. This was MY choice to write this to let people know about this amazing product.) Also, as I am writing this, there is a sale going on for this wonderful piece of heaven. I’m not a selfie person so I won’t show a picture of me on the beanbag but if you go to the website, zerogravityzen.com, you can see how much the person they have on their site loves it. I have zero (haha, get it? Zero? I know, lame. ;-) ) complaints about this. Go out and get one. Or ask for it for whatever winter holiday you choose to celebrate. Maybe for your birthday? Arbor Day? Any holiday? Any day you choose to get this amazing piece is the right day! So, go buy one and tell me what you think. I’m looking forward to hearing from you. Enjoy it in good health (and bad, if necessary)!
Nearly two weeks ago, I did a Facebook Live with Tami Stackelhouse on how to maintain a social life with fibromyalgia.
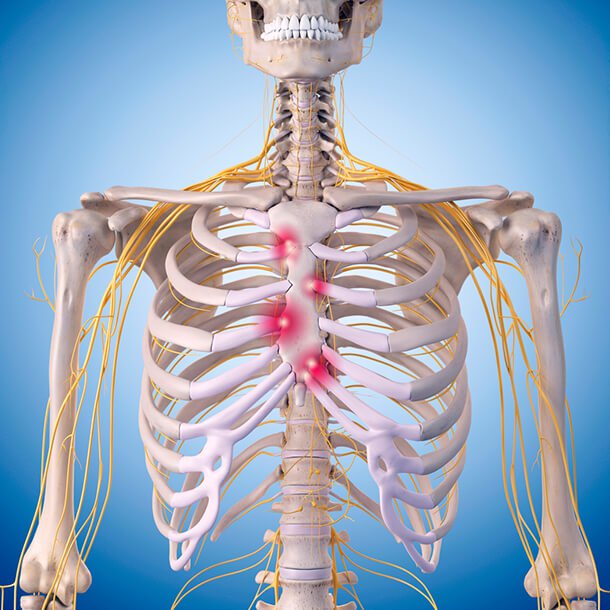
Topics include: - Learning to ask for help - How to not feel guilty - Setting realistic expectations Check it out, you might learn something!  ***Reprinted from my article on ProHealth.com published July 30, 2018.*** A couple of weeks ago, I attended a fibromyalgia coaching retreat with the International Fibromyalgia Coaching Institute. The leader of the retreat, Tami Stackelhouse, surprised us with a visit to Enso Floats in Portland, Oregon, where we could experience what it was like to receive flotation therapy. Ongoing studies of floating report physical and psychological benefits including: pain management, mindfulness, stress relief, anti-gravity effect, magnesium absorption, decreased issues with insomnia/sleeplessness, heightened senses, increased immune functions, and help with mental health disorders. According to the Fibromyalgia Flotation Project, data was collected to determine how beneficial the effects of flotation are on fibromyalgia symptoms. Below are the symptoms listed with the average amount of relief that the participants of the study reported: 66% reduction in pain level 72% reduction in being bothered by pain 66% reduction in muscle tension 66% reduction in stress levels and 66% reduction in anxiety levels. The project then reported on certain symptoms that were improved by floating including: 42% increase in freedom of movement 58% increase in energy level 64% increase in feeling of well being 163% increase in relaxation level 19% increase in amount of sleep and 83% increase in sleep quality. As someone who has heard of these benefits, I was super excited to try this potential alternative treatment to help address some of the symptoms. However, I wasn’t sure whether I would be willing to spend the money on it. Although I’m not one who likes surprises, I was thrilled with this surprise. Being given the opportunity to do this was a gift. It’s important to note though that cost is relative. According to one of my fellow coaches, though, floating would save her money, as a 90 minute float session is less than a 90 minute massage. When you walk into Enso Floats, you enter into an open room with minimalist decorations and the smell of patchouli. Also, a sweet dog greets you warmly along with the employees. Calming teas and water are available to drink before or after your floating session. (Note: Please be aware that the description of this floating center is most likely different from others around the country or the world.) Before starting my session, my fellow coaches and I were given a tour of the facility, which includes five large rooms with two circular eight foot tanks and three six by eight cabins. One of the latter cabins was an open tank helpful to those that might deal with claustrophobia. Each room had a shower with shampoo, conditioner, and soap available for use. Prior to entering the tank, we were required to shower with soap and wet our hair to wash out any products we might have and encouraged to shower after our floating session to clean our bodies of residual salt. We were given the option to leave the lights on, have complete darkness (sensory deprivation), or set lights that looked like the constellations. I chose the latter and loved it. Below is a picture of one of the circular tanks. After showering, I was eager to enter my tank. The room smelled slightly of sulfur due to the amount of Epsom salts in each tank (1,000 pounds in each tank!), but it wasn’t overwhelming or unpleasant. Having been to Israel before, I asked the employee whether the amount of salt in this water was similar to that of the Dead Sea. His response was that it was five times as buoyant. Whoa! I remember going into the Dead Sea and having trouble keeping my feet on the bottom, so I was super curious as to how this would work, especially since the tank was only filled with 18 inches of water. I placed the provided ear plugs in my ears (to keep the water from getting into my ears), stepped into the tank, picked up the head “pillow” (a foam contraption used to support your head and neck), and sat down in the water. It felt slightly slimy, but not uncomfortable, so I laid back, put my head on the pillow, let go of my inhibitions and began to float. One might think it difficult to float in only 18 inches of water but that was not the case. As you can see from the picture above, the water supports you and the only thing you need to do is find the position that’s most comfortable for you. I felt most comfortable with my legs separated a bit and out straight as well as my arms out, turning my body into a “T.” Any movement you make causes you to move, so there were several instances where I would gently bump the edge of the tank but it was not bothersome at all. Once I was comfortable in my position, I would alternate between closing my eyes and opening them to enjoy the “stars” above. For 20 minutes, I was in pure heaven. But then I began to itch. I would move a leg to “scratch” the other or use my hand to gently scratch my face or arms. It took me only a couple of minutes to understand why I was itching. It was not an issue of cleanliness. I had forgotten that I do not do well with topical magnesium treatments. I had tried magnesium in lotion and oil form previously, and it caused my legs to turn red and itch tremendously. This is what was happening here. But, I refused to let it get to me and I turned to focusing on my breath and silently reciting some meditations and mantras to get the focus off the itching. It didn’t quite work, but I did stay in the tank the entire time. Thankfully, my legs did not turn red and not long after I showered the itching did go away. Our warning signal that our session was over was a couple of minutes of quiet music and then the lights came on in the room. I got out of the tank, showered, dressed, and met my fellow coaches in the waiting room. I was one of the last to come out. Most of us expressed that we were glad to have the opportunity to try this out. Here are some anonymous quotes of how my fellow coaches felt during/after the float: “I have claustrophobia so I was concerned, but I left the doors open in the tank and I was fine. I found it to be a relaxing area. I can’t normally lie on my back but thought I’d try it with the neck/head support they provided. It felt very uncomfortable so I sat up and continued the rest of the session sitting in the tank. It did help with my lower back/leg/knee pain. However, it did result in a mini flare in my shoulder and neck area.” “I found it way more helpful than massage. The 90 minute float session was like getting the most amazing night’s sleep. I walked out of there feeling like I got a ‘regular’ person’s night’s sleep.” “It reduced my body pain significantly. I had terrible pain the day going into it and was pain free for the next two days and drastic reduction after. My mind was chattery so would not do it again for relaxation purpose but would try it again for pain reduction.” I’m not sharing these to discourage anyone from trying out the floating tanks; in fact, just the opposite. I highly recommend that anyone with fibromyalgia or other chronic illnesses try it out as there is strong research stating that the use of flotation tanks provides significant benefits (ones listed in the first paragraph), including the results of this article. Everyone with fibromyalgia (and other chronic [pain] disorders) requires a combination of different medications, supplements, and treatments. Flotation is one that has strong research to prove that it helps many. If you have any more questions about my experience, flotation therapy in general, or anything that you might need support with regarding your fibromyalgia, you can contact me here. I look forward to hearing from you soon! I volunteered for the opportunity to read and review the book entitled THE PAIN COMPANION: Everyday Wisdom for Living with and Moving Beyond Chronic Pain by Sarah Anne Shockley. In exchange for reading an early copy of the book, I agreed to review it. As someone who lives with chronic pain myself (fibromyalgia primarily), I was excited to read a book that might help give me and others perspective as in how to address our pain, accept it, and hopefully move beyond it. The author, Sarah Ann Shockley, has been suffering with chronic pain for many years. She began her book as a journal just for herself, her feelings and her reflections as she dealt with her chronic pain disorder. She realized after writing these journal entries that these reflections could not only help herself but others also living with chronic pain. While our chronic pain diagnoses are different, I identified with a lot that she went through and appreciated the reason for the book. What I also really liked within the book was that at the end of each chapter, Sarah Anne shared an outline of a quick review of that chapter’s most important takeaways Another thing I really appreciated about Sarah Anne’s book in her persistence in making sure the reader knows that they are not alone in their suffering. People with chronic pain disorders, while they might have different disorders, can connect with the pain component alone. The way she addresses pain is different from most. As a coach for people with fibromyalgia, I can see some reading her book and jumping on the “I can do this!” bandwagon, and others feeling like they’ve gone through too much (even thinking they’ve done what Sarah Anne talks about in her book and aren’t interested in trying something potential new. I always encourage my clients to step out of their safe zone to address the things they need help with most and I see the author doing the same thing. I would recommend this book to anyone living in pain, loving someone in pain, or has lost someone due to their pain. I think this book is written to address people living in different stages of pain as well. Kudos to Sarah Anne for sharing her own experiences and life lessons to help others! About a week ago, I noticed some lower back pain and slight pain around the back of my rib cage. I initially attributed it to a fibro flare due to the fluctuations in weather that Pittsburgh has had lately. I treated myself with ice packs and pain meds but nothing seemed to work. In fact, the pain increased and spread. I started noticing sciatica down my left leg and increasing pain in my ribs both front and back. This happened to me two years ago (as I was reminded by my chiropractor at my appointment yesterday) but I let the pain get really bad before I checked in with my PCP. I just figured it was a really bad fibro flare and that I would rest, ice, and take ibuprofen (no other pain meds at that point) and it would go away, but it didn’t. I went to see my PCP who noticed the inflammation in my back to the point where my back was warm to the touch. She tried trigger point injections but they barely touched the pain. I was referred for an MRI scan to see if there was anything wrong and the scan showed nothing. Someone suggested seeing a chiropractor so I asked my PCP for a recommendation and made an appointment. I got to this appointment apprehensive and slightly scared as I’d never been to a chiropractor before and “adjustments” sounded scary and painful to me. I filled out a complete health history and the doctor checked me out. She found that (be prepared to cringe) that the reason for my pain and inflammation was due to the fact that every single one of my ribs were out of place and I had something called costochondritis. Symptoms of costochondritis include: - Inflammation of the cartilage that connects the ribs to the breast bone - Sharp, aching or pressure like pain - Causes difficulty in taking big breaths as it worsens the pain Currently, costochondritis has no specific cause. It just causes intense pain. I am sitting here with an ice pack strapped to my back. During yesterday’s appointment, the chiropractor noticed that some of my ribs were out of place (AGAIN) and my hips were misaligned. She made some adjustments and nearly instantly most of the pain has disappeared. When I went two years ago, it took several appointments plus a script from my PCP for a prescription painkiller to help me function “normally” again. Surprisingly, about an hour after I returned home from my adjustment, the pain returned in full force. I have a follow up appointment on Monday. I’ll let you know how it goes. Unfortunately, costochondritis is a common co-morbid diagnosis with fibromyalgia. What this means is that it is not uncommon to have costochondritis alongside your fibromyalgia. There are different types as well. There is chronic costochondritis which means it comes back with some sense of regularity and there is a one time type as well. Also, the level of pain that you experience can be different. I’ve had times with my chronic costochondritis that the pain was manageable and an appointment to the chiropractor was not needed. But, the point here is that when we have fibromyalgia, we often just automatically blame new pain on the fibro. However, the pain isn’t always related to fibromyalgia. So, if you notice pain in a new area, I highly recommend going to see your doctor to see if there might be something else going on. Also, I recommend going as soon as you notice the pain -- waiting like I did two years ago was NOT the best choice. If you have questions about costochondritis or other fibro related questions, feel free to reach out. I’m always available to chat and eager to help. The best way to reach out to me here or you could email me at [email protected]. I look forward to hearing from you, speaking with you, and helping you out with those pesky fibro (or other comorbidities)! =) “No one really knows precisely what causes the debilitating fatigue and muscle pain of fibromyalgia. But some people who have the disorder say they know what can make it worse: changes in the weather. Cold, damp days and drops in barometric pressure are widely associated with flare-ups in symptoms of the condition, which affects mostly women. In one study by the National Fibromyalgia Association, people with the condition ranked weather changes as one of the leading aggravating influences on pain and stiffness.” The above quote was taken from an article written in the New York Times, in 2013. You can find the article here. I don’t know about you, but when I talk with my friends and colleagues with fibromyalgia, that is one of the major things we agree on: how we can tell the weather before the weather happens (which I hear people with arthritis report the same thing). So, you would think that because our bodies start to ache and our fatigue and fog increases that there is a connection. However, as of now, there is no research that confirms this theory! There have been articles about temperature sensitivity and body temperature dysregulation, yet nothing on the connection between barometric pressure and fibromyalgia flares. In a report in the journal Arthritis Care and Research, Dutch researchers followed over 300 women with fibromyalgia and concluded that while “weather variables had ‘significant but small’ effects on pain and fatigue...for the most part, they concluded, there was “more evidence against than in support of a uniform influence of weather on daily pain and fatigue.” Doctors that treat fibromyalgia encourage us to listen to our bodies when it comes to the three major “pieces” of fibromyalgia: pain, fatigue, and fog. However, while listening to our bodies with regard to changes in barometric pressure, we are told that there is no likely connection. So, why is it then that we can often accurately tell when there will be changes in the barometric pressure?? We may not have the answer yet but we can do things in advance to prepare for these changes. Often times, the local weather channel will alert you to changes in weather. While your body may be alerting you as well, here are some suggested precautions to help make the transition that you know your body will feel regardless of what scientific research says:
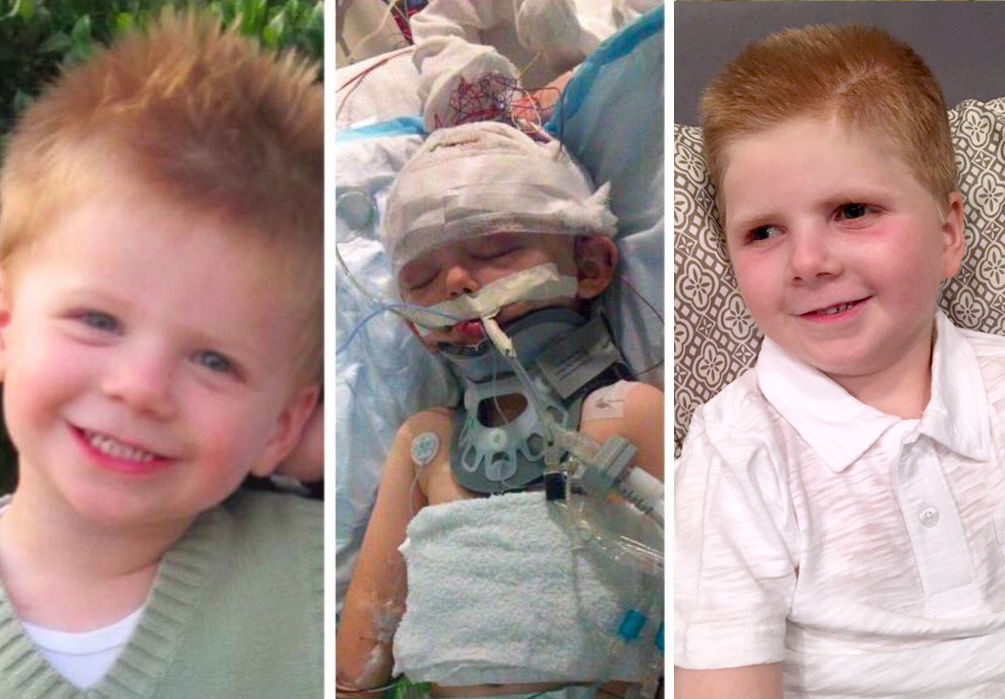
If you’ve done all you can to prepare for significant weather changes and your body is still screaming, consider a hot bath or heating pad, or if the heat bothers you, an ice pack. Allow yourself time to rest, be kind to your body, and allow yourself to feel. If you fight the symptoms, there is a good chance they will just increase in intensity. Do you need some help to figure out temperature regulation or other tips to help your fibromyalgia body during especially difficult weather transitions? I have an arsenal of ideas. I’d be happy to help you. Please feel free to drop me a line here or schedule your free consultation here. I’m happy to help assist you with any questions you have about living a life with fibromyalgia or other chronic pain disorders - and I’m happy to help you with other concerns, not just the weather! I look forward to hearing from you soon! =) Seven and a half years ago, a perfect little boy named Tripp Halstead was born. Two years later, in a freak accident on a windy day, a massive tree branch snapped and fell on Tripp’s head crushing his skull and causing much of his brain to die. Soon after that horrible incident, Tripp’s mother Stacy began a page in Tripp’s honor, posting nearly daily for five and half years about the mountains and valleys of now having a child with a Traumatic Brain Injury (TBI). On March 15, 2018, sweet Tripp’s little soul left his body for loftier places. He had been sick all winter and according to his mother, his little heart just gave out. While living with a TBI can be rather unexpected regarding illnesses, quality of life etc., Tripp’s passing was a surprise to most. Why am I sharing this? Well, I followed Tripp’s page almost from the beginning. I waited for Stacy’s post on her beautiful little boy and rejoiced in his successes and cried during his struggles. I became emotionally invested in a family that I never met. After many tears and thought processes, I realized how much Tripp taught ME about living life with a chronic illness/disorder. Resilience While Tripp was in the hospital after the accident, the doctors told his parents that he was most likely not going to survive this trauma, and that they should say goodbye. Can you even imagine what that’s like? Not only did Tripp prove the doctors wrong; but, he made improvements that were unlikely to happen due to so much trauma to the brain. As people living with fibromyalgia, we display our abilities to be resilient on a daily basis. We push through our pain, our fog, and many other symptoms under the fibromyalgia umbrella. We put on a smile for others while often struggling with crippling pain. We choose to remain positive as despite the difficulties of living with a chronic pain disorder, we know things can be much worse. We learn strategies to address the most difficult manifestations of our disorder. Strength Tripp endured ridiculous levels of pain due to his skull literally being crushed causing severe trauma to his brain. Even with copious amounts of pain medicine, his brain (the part that was still alive) was misfiring and swollen causing the rest of his body to swell, also causing pain. But something in the part of Tripp’s brain that was still working pushed his body to fight what was supposed to be inevitable. He spent so many months in the hospital and was a shell of the toddler he was before; but, nonetheless came home and in the five years after the accident, and made small but incremental improvements. Strength is something we need to focus on and fight for daily. Living with the symptoms that we do, not only do we rely on physical strength to get things done, we rely on the mental strength to push us to use our physical strength. Being in pain, being foggy, having the inability to focus are all common symptoms of fibromyalgia. As part of our strength, we need to figure out (on a daily basis) where we want to focus our strength. We also need to reserve our strength for those days where our symptoms are at their worst. This is where we use (or save) our spoons. For those of you not familiar with the Spoon Theory, you can read about it here. Persistence Tripp was a fighter. Despite the many obstacles he faced, he persevered. He learned ways to communicate again, he learned to smile, he learned to move his body, he learned to protest. All of these are things we take for granted but Tripp had to relearn everything. Chances are that if he lived a longer life that his life would never go back to what it was before the accident but improvement is improvement. Despite the pain, the many surgeries, all the therapies, etc., Tripp persisted. He showed improvements. He showed that somewhere, the “old” Tripp was still in there. Persistence is something that we, as fibro warriors, need for us to continue. An initial diagnosis can be upsetting, frustrating, angering but once you move past the mourning period, you come to realize that life is different but it doesn’t mean that life will be bad. Persistence is how we get up in the morning. It’s how we go to work, or care for a family. The last thing we want to do is give up as allowing your body to “succumb,” for lack of a better word, to our illness. Will we struggle? Yes. Will it be hard? Yes. But there are strategies, activities, medications and supplements that can help us fight this illness and work on living a happy and full life. For the most part, Tripp was a happy little boy who just happened to have a traumatic brain injury. His life would have been drastically different had the branch not fallen on his head but something in Tripp kept him fighting for as long as he could. As we live with chronic pain and other chronic disorders, we need to keep in mind, and in perspective that things could truly be much worse. If you are struggling with finding your “happy place,” reach out to me here. I have an arsenal of suggestions that could make life living with a chronic pain disorder much easier. For the most part, I live a life of low pain, reduced fog, and the ability to help others living with fibromyalgia and other chronic pain disorders. Take advice from Tripp (may his memory be a blessing to his family and followers). Obstacles do not have to prevent you from living a happy and full life. I look forward to hearing from you soon! =) As many of us fibromites know, food can help with healing, or it can be our kryptonite. Each person with fibromyalgia may have different sensitivities or allergies to a variety of different foods, but may not know it until the proper testing is done. Sometimes though, testing doesn’t NEED to be done as your own body will tell you whether or not it can handle the food you ate. Several years ago, I was put on a diet due to the fact that I had something called SIBO (Small Intestinal Bacterial Overgrowth). Sounds gross, right? Well, everyone has bacteria in the intestines to help with digestion but because I was eating a significant amount of carbs and processed sugar, “bad” bacteria was growing, causing symptoms similar to and intensifying my fibromyalgia symptoms. After going on a major diet change including: low carb, high fat, very little dairy, few fruits, selected vegetables, gluten free, you get the idea. For this kosher picky vegetarian, it was HARD! But, after the withdrawal symptoms were over, I began to feel GOOD. My pain decreased, my fog decreased, and most of my fibro symptoms decreased. It felt like a miracle! But, I did this diet for three months, my SIBO went away, and my naturopath (who diagnosed the SIBO) stated that it was gone. Noticing that I was feeling better, I took it upon myself to remain gluten free and processed sugar free and since then, my fibro symptoms are much better managed than they were before my SIBO diagnosis. But, why do I bring this long-ish story up? Because even in the non-fibro world, going gluten free and processed sugar free has become a “thing.” It’s become popular and people notice that without eating the processed junk, eating a whole foods (and I don’t mean the store) diet, people had more energy, were able to focus better, and much more. Also, studies have shown that there is a high incidence of SIBO in people with fibromyalgia They will often go undiagnosed as many Western doctors do not even know what it is. As I stated before, I was diagnosed by my naturopath. Many of the clients that I have seen have either also been on a gluten free, refined sugar free diet, or had a list of food allergies/sensitivities that made going on the above diet make the most sense. As their advisor, I have been able to successfully transition many of my clients to food plans that work well with their health concerns. And after many weeks on said food plan, many reported that they noticed a decrease in their fibro symptoms. So, do you have to change what you eat in order to feel better? Dr. Ginevra Liptan (a doctor who treats fibromyalgia while living with fibromyalgia) made the following statement in an article on WebMd, that discussed fibromyalgia and diet. She noted “There aren't many good studies that have looked at how diet can affect fibromyalgia symptoms. But I think we can gather a lot from anecdotal evidence -- from what patients tell us," says Ginevra Liptan, MD, medical director of the Frida Center for Fibromyalgia in Portland, Ore., and author of Figuring Out Fibromyalgia: Current Science and the Most Effective Treatments.” Basically, trust your gut. Are you struggling with digestive issues alongside your fibromyalgia? Well, you’re not alone. IBS (Irritable Bowel Syndrome), SIBO, GERD (Gastroesophageal reflux disease) are all common. Interested in getting some help to address these concerns? Well, over the counter medications like Prilosec can help, but most likely what you’ll need to do is change your diet. This is something that a Fibromyalgia Coach/Advisor can help you with. As I said before, I’ve worked with many clients on these issues and they have been pleased with their results. Why not set up a free consultation and we can talk about what we can do to help your fibromyalgia and digestive concerns. You can contact me here or schedule a consultation directly here. I look forward to hearing you soon! In the meantime, find that food that nourishes your body and your soul. It’s out there, I promise. =) Ed Coghlan, author of an article with the same title as the one above, discusses how pain patients are being punished for the so called opioid crisis when the problem isn’t the patients themselves. He quotes Dr. Jay Joshi, one of the leading pain physicians as saying “This deeply misguided, if predictable, response threatens to deprive millions of Americans of relief from persistent, even debilitating pain. Instead of retreating from treating their pain altogether, we should focus on educating doctors on the multitude of safe, effective methods for treating pain in its various forms.” Clearly the opioid crisis is a big issue of contention between the CDC, pain patients, and their doctors. Doctors that prescribe opioids for their patients are receiving significant pressure from the CDC to decrease or even completely remove the opioid medication from chronic pain sufferers treatment plans. Because there is an apparent overuse of opioids to get high, the CDC believes this is the only way to stop the “crisis.” Dr. Joshi has another idea that makes sense. In an article he authored in November 2017, Joshi stated that “we should start by creating a set of standard guidelines or recommendations (a framework), like the compendiums that exist in every medical specialty, for pain treatment... The lack of any such a framework is largely responsible for creating the opioid crisis. Lacking a useful set of standards for treating pain, and under pressure to treat pain by federal standards, insurers and professional associations, physicians over-prescribed the only treatment they understood. Some drug companies exploited that knowledge gap, convincing lazy or unsophisticated physicians that opioids were the answer for all kinds of pain–and even, in some cases, that opiates weren’t addictive.” So, who do we blame for the opioid crisis and how do we address the issues so that pain patients can be treated in the most effective way? Joshi suggests that we “don’t blame opiates for the opiate crisis. Stupidity and laziness among my fellow physicians play a role, as does opportunism by certain opioid manufacturers.” He also states that “we can reverse the damage, and prevent the further spread of addiction. But we must educate doctors on the array of available avenues for treating pain, and provide them with a clear framework for which avenue work best for which ailments.” Dr. Joshi does admit that opioids are not for everyone; however, if treatment for chronic pain with opioids works in someone who does NOT have an addiction issue, that treatment should not be stopped as it punishes the patient for something that is not their fault. There are apparently “no residencies offered in pain management and estimates that 90% of the “pain specialists” in America have no formal, accredited fellowship training in pain management.” My Opinion I agree with Dr. Joshi. Chronic pain patients like us are being punished for an issue that most of us do not deal with: addiction. There is a difference between needing pills to manage your pain versus using the pills to get high and obliterate all feelings that you have. So, there are two issues that need to be addressed. First, there needs to be a program in medical school or a residency that specifically focuses on pain management and possibly has a focus within that that addresses how to use pain management with people that live with chronic pain. Secondly, while I don’t agree with how the CDC is addressing the “opioid crisis,” I do agree that addiction is a major issue in this country that needs to be addressed. Maybe the CDC and medical programs/residencies can work together so that doctors can learn to identify the difference between an addict and someone who needs these meds to control their chronic pain. With this training, there can be a certain amount of control on the prescribing of opioids as regularly as they might be prescribed and the issue of addiction can be addressed as well. (Addiction is an entirely different topic that I don’t have enough experience or knowledge of but that absolutely needs to be addressed.) What I also know is important is that doctors shouldn’t be shamed for prescribing these medications and patients shouldn’t be ashamed to take them. There has got to be a “happy medium” for lack of a better term. I’d love YOUR opinion on the topic. Please feel free to comment below or send me a private message here (on my website) or here (on my Facebook page). If you are interested in coaching, interesting in learning about another topic, please let me know! My goal is to help as many people live life to their fullest while living with a chronic illness. Sign up for a FREE consult. There are no requirements to continue past that point to learn what coaching is all about and how much it can benefit your life while living with fibromyalgia. I look forward to talking with you soon! |
AuthorI’m Kate Straus and I’m a Certified Fibromyalgia Advisor. I help Jewish women feel confident in their ability to practice their faith while navigating the ups and downs of fibromyalgia. I’m using the disease that at one time knocked me down, to help support others live life to their fullest. Archives
January 2021
Categories |






 RSS Feed
RSS Feed


